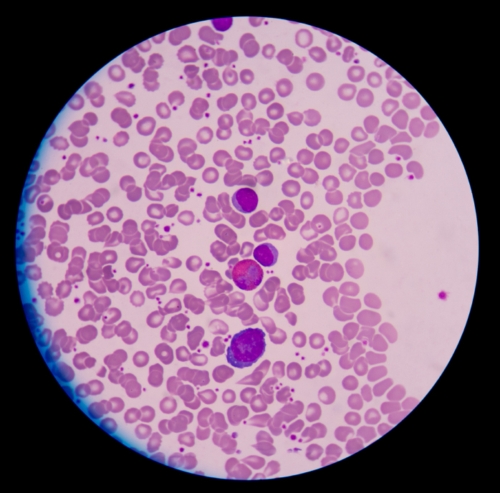
 The good news is that the treatment sent roughly 90% of patients with terminal leukemia into remission. The bad news is that it may have killed two and sent others into intensive care. These yet-unpublished findings were presented to the annual meeting of the American Association for the Advancement of Science and offer a potential treatment of last resort for otherwise hopeless cancer cases—assuming the kinks get worked out.
The good news is that the treatment sent roughly 90% of patients with terminal leukemia into remission. The bad news is that it may have killed two and sent others into intensive care. These yet-unpublished findings were presented to the annual meeting of the American Association for the Advancement of Science and offer a potential treatment of last resort for otherwise hopeless cancer cases—assuming the kinks get worked out.
The treatment revolves around the body’s T-cells, a form of immune cell that works sort of like a bomb by targeting infectious tissue and destroying it. Scientists from the Fred Hutchinson Cancer Research Centre in Seattle devised a method that would reprogram the means by which T-cells find their targets, effectively customizing them to target the patient’s cancer.
This customization was accomplished by using genetic encoding to add what is called a “CAR19” receptor, allowing the T-cell to identify and react to the CD19 protein, which is found on cells composing lymphomas and leukemias.
The trial covered 29 people with an advanced and fatal form of leukemia that had been unresponsive to other forms of treatment. Without another option, every patient was terminal. Impressively, a single dose of the T-cell reprogramming treatment sent 27 of the patients into full remission. The cure was so complete that the scientists were unable to detect leukemia cells within their bodies. Good news, certainly, but there were also complications.
Seven patients experienced what is known as “cytokine release syndrome”, a severe and rare full-body inflammatory response that sent the victims into intensive care. Two others also died from complications relating to the treatment. While these results could in some ways be considered acceptable—the alternative was all 29 facing untreatable, terminal cancer—but these side effects currently make the treatment highly inadvisable for general use. Conventional leukemia treatments have much less severe side effects and continue to work on most patients.
Future research on the treatment will look into ways to minimize and reduce the dangers to patients. Investigation will also need to be done to see how other types of cancers respond to the treatment, not just leukemia. Of particular interest will be how the treatment behaves against more solid-type tumors, such as those found in breast cancer.
Leukemia, being a cancer of the bone marrow, creates tumors out of softer tissue that may be easier for the modified T-cells to attack. Regardless, however, these findings are an impressive step forward for the field of immunotherapy treatment and offer hope for future developments.
Sources for Today’s Article:
“Abstract: Engineering T Cells for Safe and Effective Cancer Immunotherapy (2016 AAAS Annual Meeting (February 11-15, 2016),” AAAS 2016 Annual Meeting. February 14, 2016; https://aaas.confex.com/aaas/2016/webprogram/Paper16827.html, last accessed February 17, 2016.
